What is Self-care?
Self-care is about looking after yourself in a healthy way. It can be anything from taking care of your teeth, doing some exercise, managing common conditions (like headaches, colds and flu) or living with a long-term health problem, such as asthma or diabetes.
As a Self-care promoting practice, we are here to help you feel able to look after your own health when it is right for you. So, when you come in for a consultation, the doctors, nurses and healthcare assistants in this practice will talk to you about what you can do to help maintain and improve your health.
Self-care for healthy living
Staying healthy is important for everyone, even if you are living with a long-term condition. This means eating healthy, exercising regularly, quitting smoking and drinking in moderation.
If you are not sure what changes you can make to help improve your health, NHS offers advice on Living Well. Click here for access to the Live Well Hub.
Find out more about self-care for healthy living
NHS provides lots of useful information on how you can improve your health and well-being. Click on the links below to find some of the examples:
Self-care for common conditions
Did you know that one in five GP visits are for common conditions, such as backache, headache or cough?
For most people, they are not serious health problems – you just want to know how to relieve it and you want a treatment that acts fast. You also want to know how long you’re going to suffer or what you should do if your symptoms change.
The good news is that self-care can help you manage most of these problems. It may mean you don’t have to spend time waiting to see your GP but can get on and start tackling your symptoms. Self-care for common conditions can also help free up some of your GP’s time, making it easier to get an appointment when you have a more serious condition.
Find out more about self-care for common conditions
The Self-care Forum has produced Factsheets to help you take care of the most common ailments. These provide useful facts about your condition, what you can expect to happen, how to help yourself, when you should see your GP and where to find out more information. Research shows people using these Factsheets felt more able to manage their common condition.
Click on the links below for the Factsheet you need:







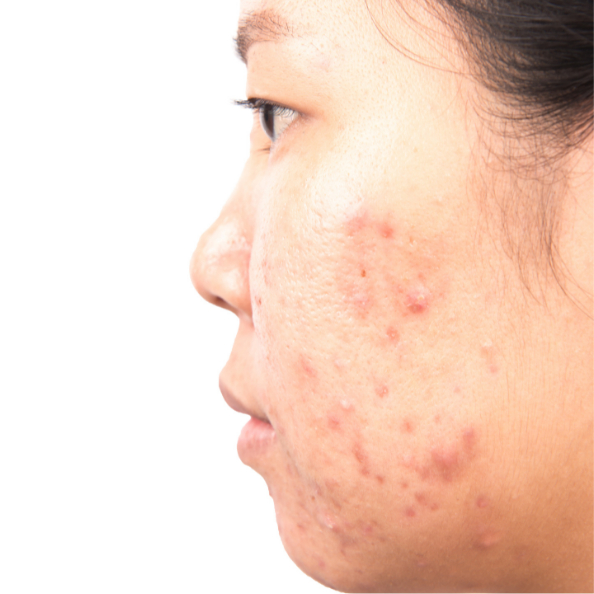
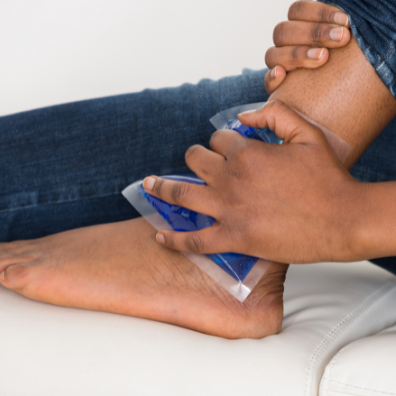





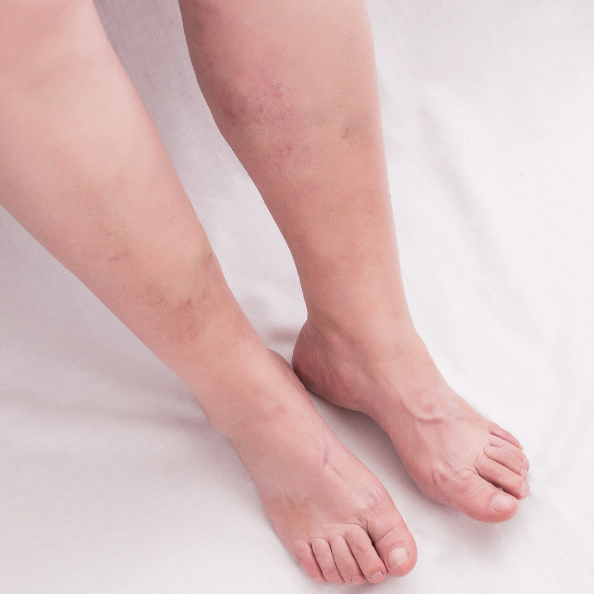






If you need more advice or you are unsure what the right thing for you to do is, ask your pharmacist for advice or call the medical centre to speak to a doctor or make an appointment to discuss your problem further.
Self-care for long-term conditions
Did you know that if you are living with a long-term condition, you will spend, on average, six hours a year with a healthcare professional and the remaining 8,754 hours managing your health yourself?
Living with a long-term condition brings challenges and it’s important to have the confidence, support and information to manage your health. Self-care can help you make the most of living with your condition, rather than avoiding or missing out on things because of it. Self-care puts you in control.
Research shows that people with long-term conditions who take more control of their health feel more able to cope with their health problems, have better pain management, fewer flare-ups and more energy.
We are committed to helping you live your life with a long-term condition. That’s why we run services where you can get advice on the following conditions:
- Asthma
- Diabetes
- Chronic conditions
Taking your medicines regularly is an important part of keeping yourself well. Many people have problems taking medicines such as remembering to take them at the right time and side effects. Speak to your pharmacist or practice nurse and they will be able to help you. We will also work in partnership with you to create the right care plan for your needs. It’s important to think about what you want from a care plan – it can help if you know what you want to discuss with your GP. NHS suggests some questions you could ask:
- Where can I find out about self-help courses for people who have long-term conditions?
- I want to find out more about my condition. What are the best places to do this?
- Is there any new equipment that might help me manage day-to-day? If so, how do I get it?
- How do I meet other people who have the same condition as me? Is there a local or national support group?
- What support can I get to help me take my medicines
- Are there any lifestyle changes I should make to help my health, such as giving up smoking, avoiding certain foods, or doing more of a certain type of exercise?
- What are the results of my tests and what do they mean for me?
- What happens next?
- What can I do?
- What can the doctor do?
Tips for living with a long-term condition
- Accept you have a persistent health condition…and then begin to move on
- Take your medication as prescribed – if you have any problems with your medication ask your pharmacist
- Get involved – building a support team
- Pacing – pacing your daily activities
- Learn to prioritise and plan your days
- Setting goals/action plans
- Being patient with yourself
- Learn relaxation skills
- Exercise
- Keep a diary and track your progress
- Have a plan for set-backs
- Teamwork – work with your practice team
- Keeping it up
Find out more about self-care for long-term conditions
There is a range of free courses aimed at helping people who are living with a long-term condition to manage their condition better on a daily basis:
- DAFNE (Dose Adjustment for Normal Eating) and DESMOND (Diabetes Education and Self-Management for Ongoing and Newly Diagnosed) for people with diabetes
- Breathe Easy for people with asthma – click here for information
These courses usually run over several sessions and will provide advice and tools to put you in control of your condition. Ask your GP or the receptionist for details of courses in this area or visit the NHS website. Click here for more information.
Self-care ideas to get you started
Post work wind down
Long days or nights whilst training can take a toll on the mind and body. Some people enjoy having a post-work wind-down routine. Do you have a routine that works well for you? What do you do to wind down after work?
Nourish the mind and the soul
Some people find spending time in the kitchen therapeutic, which is an added bonus if you see it as self-care time. Making food to nourish your mind, while winding down after a day at university or in the department is beneficial.
Keep hydrated
Keeping hydrated is also an important part of self-care because without water we can feel tired, leaving little energy left after studying and work. Many learners report that as soon as they started the habit of drinking water daily, it became second nature. Here are some ideas on how to keep hydrated whilst working or studying.
- start the day with two cups of warm water
- set your own goals of how much you want to drink in a day and aim to reach that goal
- infuse your water with lemon, ginger, cucumber, and mint
- juicing is a great way to ensure you take more fluids
- set times throughout the day that you would like to have drank a certain amount by, e.g. 1 litre every 4 hours
- keep a bottle or cup of water, or juice, in front of you at all times to remind you to drink
- use a motivational bottle to help keep up with drinking that has written reminders on the bottle when to drink
- change your water bottle to a new one every so often and make sure it’s one you like looking at as it may encourage you to drink more
Sleep well
Sleep is a vital part of self-care. A lack of sleep can affect concentration, weaken your immune system, and make you more accident-prone, amongst other issues. Trainees sometimes find it hard to wind down after a long day. It’s advisable to find a routine that works for you that helps you find a way to go to sleep at night. Here are a few ideas that may help you drift off into a peaceful sleep.
- meditate
- hydrate before going to bed
- exercise
- relaxing shower or bath
- cup of Chamomile tea
- don’t use the phone an hour before sleep
- lavender on the pillow
- use an eye mask
- make sure your sleep space is tidy
- write down any notes for the next day to help clear your mind
- read
Take time out for you
It’s easy to get caught up in university life, impending assignments, or work-based learning. Some people have long journeys at the start and end of the day, and use that time to catch up with friends, read a book or listen to music. Finding a way to fit family and friends into your life can be difficult, but it’s important to carve out time for people close to you as they are your support system.
Once you’ve found some time for yourself, what can you do with that time to ensure self-care is a part of the experience? Here are a few ideas. These can be done alone or with others. But whatever you do, make the most of your time.
- nature walks
- arts and crafts
- shopping
- cooking
- listening to music
- going to the cinema
- spending time with family and friends
- exercise
- meditation
- sleeping
- driving
- travelling
- spa days
- gardening
- volunteer work
- watching sports
- bowling and many more
Be prepared to make over your medicine cabinet
Coughs, colds, headaches and other common illnesses can leave you feeling unwell and struggling to carry on as normal. Be prepared by keeping a well-stocked medicine cabinet at home.
All it takes is just 5 minutes to make sure your medicine cabinet is ready to help you manage common illnesses. GPs recommend your medicine cabinet should contain the following:
- A self-care guide
- Painkillers, such as paracetamol or ibuprofen
- Antihistamines for allergies
- Antiseptic cream for bites and stings
- A laxative to help constipation
- Sunscreen
- A first aid kit with plasters and bandages to manage cuts and sprains
Always be careful to follow the product instructions and regularly check medicines if they are not expired. If you’re not sure what medicines to stock or how best to treat the symptoms of common health problems. Ask your pharmacist for advice.
Minor illness
Common ailments can often be treated by yourself at home using medicines that are available over the counter from your local pharmacy (chemist) or supermarket. NHS 111 can provide advice on their website or on the phone and your local pharmacist can also advise you on minor illnesses.
Every year, millions of us visit our GP with minor health problems that our local pharmacist could resolve.
It is estimated that every year 50 million visits to the GP are made for minor ailments such as coughs and colds, mild eczema, and athlete’s foot. But by visiting your pharmacy instead, you could save yourself time and trouble.
Instead of booking and waiting for a GP appointment, you can visit your local pharmacist any time: just walk in.
All pharmacists can recognise many common health complaints. They can give advice or, where appropriate, medicines that will help to clear up the problem. If your problem is more serious and needs the attention of a GP, your pharmacist will recognise this and advise you to see your GP.
What’s more, many pharmacies are open in the evenings and on the weekends.
If everybody went to a pharmacist with common health problems, more time would be freed for our GPs. This might make it easier to get a convenient appointment with your GP next time you need one.
So if you have a common health problem, a trip to your pharmacy is an option.
Your pharmacist may be able to help with:
- skin conditions, such as mild acne and mild eczema
- coughs and colds, including nasal congestion and sore throat
- minor cuts and bruises
- constipation and haemorrhoids (piles)
- hay fever and allergies
- aches and pains, such as headaches, earaches and backache
- indigestion, diarrhoea and threadworms
- period pain and thrush
- warts and verrucas, mouth ulcers and cold sores
- athlete’s foot
- nappy rash and teething
Some pharmacies can provide truss fittings, stoma products and incontinence supplies.
Go to your GP, a walk-in centre or accident and emergency for:
- suturing or wound and dressing care
- muscle and joint injuries, including strains and sprains
- lacerations, cuts, fractures, severe sprains and strains
- infected wounds and foreign bodies
- head injuries or loss of consciousness
- suspected broken bones or heavy blood loss
- persistent chest pain or difficulty breathing
- overdose or poisoning
Minor ailment services
Some pharmacies run a minor ailment service, which means that they can supply medicines for certain specific conditions on the NHS. It’s up to local primary care trusts (PCTs) to decide whether pharmacies in your area provide these services.
If your pharmacy runs a minor ailment service for eczema, for example, it means that your pharmacist can supply medicines for this condition, and you’ll only pay the standard prescription charge. Or if you’re exempt from paying prescription charges, for example, because you’re over 60, you won’t pay for the medicine.
Use service search to look for pharmacies in your area or simply ask at your local pharmacy.
Useful links: